What is atopic dermatitis?
Atopic dermatitis, also known as atopic eczema, is a chronic inflammatory skin disease characterised by recurrent flare-ups of intense itching, dryness, and redness. It is not simply "dry skin"; it is a complex immune system condition that affects the skin barrier and, in moderate to severe cases, profoundly impacts sleep quality, mental health, and the daily performance of those who suffer from it.
Fast-track your treatment
To book an appointment or speak to a member of the team, please contact us using the following options.
Why does it appear?
→ Genetic causes and environmental factors
It is not a choice; it is biology. There is a strong hereditary predisposition: if your parents suffer from asthma, allergic rhinitis, or eczema, your chances of developing atopic dermatitis increase significantly. However, environmental factors act as the "switch" that triggers the inflammation:
- Urban pollution: Airborne particles can penetrate weakened skin.
- Climate and heating: Sudden temperature changes and dry indoor air draw moisture out of the dermis.
- Emotional stress: Although it is not the primary cause, stress releases cortisol and other substances that exacerbate itching.
→ Skin barrier dysfunction: the role of filaggrin
In atopic dermatitis, there is often a deficiency of filaggrin, an essential protein for the skin's structure. This causes the barrier to become porous: water escapes (causing dehydration) and allergens or bacteria enter easily, triggering your immune system to generate the inflammation you see and feel.
Main symptoms: How to identify atopic eczema?
| Life stage | Typical location | Type of lesion |
|---|---|---|
| Infants (0-2 years) | Cheeks, scalp, and extension areas (elbows/knees). | Red, "weeping" lesions (with exudate) and scaling. |
| Childhood (2-12 years) | Elbow creases, popliteal fossae (behind knees), wrists, and ankles. | Very dry, thickened skin (lichenification) and scratch marks. |
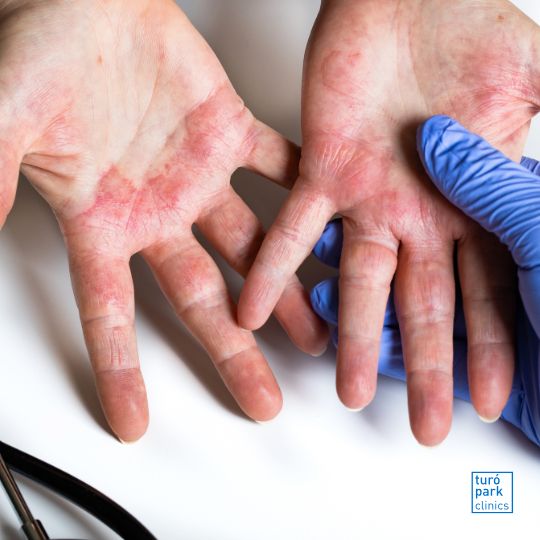
| Adults (>12 years) | Face, neck, neckline (décolletage), hands, and limb flexures. | Dry, very thickened, and grayish patches. High impact on visible areas. |
We take care of your skin.
Our dermatologists welcome you for personalised care of all your skin, hair and nail concerns.

Differential diagnosis: Is it dermatitis, psoriasis, or an allergy?
One of the greatest challenges is the patient who arrives self-diagnosed. It is fundamental to understand that not every red, itchy skin condition is atopic dermatitis. An accurate diagnosis by a specialist is the first step toward successful treatment. There are three conditions that are frequently confused:
→ Atopic Dermatitis
It is defined by intense itching, a family history of allergies, and lesions in the flexures of the elbows or knees. The skin is extremely dry.
→ Psoriasis
Unlike dermatitis, psoriasis patches are usually very well-defined, have a thick whitish or silvery scale, and typically appear on the elbows, knees, and lower back. The itching is usually less intense than in atopy.
→ Contact Dermatitis (Allergy)
It appears suddenly after touching a specific substance (such as nickel, perfumes, or certain cosmetic preservatives). The lesion is limited to the area that touched the object.
Distinguishing these pathologies requires a meticulous clinical inspection and, occasionally, patch tests or skin biopsies to confirm the diagnostic suspicion and avoid wasting time with creams that will not work.
Treatments for atopic dermatitis
During the consultation, a specialist applies precision medicine to stop inflammation at its molecular source. Depending on the severity of your condition, we offer a range of treatment options designed to restore your quality of life:
Narrow band phototherapy (UVB-B) uses light waves to 'calm' the immune cells in the dermis. It is safe, non-invasive and ideal for those who do not wish to take oral medication.
For moderate to severe dermatitis, biologics have transformed the prognosis. Dupilumab is a monoclonal antibody that acts like a 'precision key': it specifically blocks the interleukin (IL-4 and IL-13) receptors responsible for type 2 inflammation. Unlike older immunosuppressants, it does not affect the entire immune system, offering exceptional safety.
The latest innovation is Janus kinase (JAK) inhibitors. These oral treatments are ideal for:
- Extremely fast-acting: Itching can be significantly reduced in just 48-72 hours.
- Convenience: Perfect for patients with a fear of needles who prefer to avoid injectable biologics.
- Complete control: They enable almost complete remission in very resistant cases.
Tips for daily life and preventing flare-ups
Medical treatment accounts for 50% of success; the other 50% depends on what you do at home.
- The 3 minute rule: Apply your moisturiser immediately after showering, whilst your skin is still slightly damp, to 'lock' the water into your skin cells.
- Showers, not baths: The water should be likewarm (never hot) and showers should last no longer than 5-10 minuted. Use syndet (soap free) gels.
- Natural fabrics: Prioritise organic cotton, linen or silk. Avoid wool and synthetic fibres that trap sweat and trigger itching.
- Controlling night time scratching: Keep your nails short and clean. If the itching is uncontrollable at night, wearing cotton gloves can prevent injuries from involuntary scratching.
Our multilingual dermatologists




Our answers to the most frequently asked questions about atopic dermatitis
Can atopic dermatitis be permanently cured?
It is a chronic condition, so there is no single "cure." However, with new biological and oral (JAK) treatments, we achieve complete remission: many patients enjoy years without flare-ups or itching.
Is atopic dermatitis contagious?
Absolutely not. It is a genetic and immunological disease. The marks and scaling are signs of internal inflammation, not a transmissible infection.
Can I play sports if I have a dermatitis flare-up?
Yes, but with caution. Sweat irritates atopic skin; wear breathable clothing, shower with lukewarm water immediately after, and apply moisturizer to restore the skin barrier.
Does stress influence the appearance of flare-ups?
Stress does not cause dermatitis, but it is a powerful trigger. It releases inflammatory substances that weaken the skin's defenses and increase sensitivity to itching.
Is long-term use of topical corticosteroids safe?
They are useful for stopping acute flare-ups, but prolonged use can cause skin atrophy. Our strategy is based on steroid-sparing agents and modern systemic therapies to avoid side effects.

Dr. Luis Novoa is a renowned specialist with dual board certifications and over 10 years of experience. An expert in diagnosing and treating skin conditions, STDs, and systemic diseases, he combines clinical practice with teaching at the CTO Group and international scientific research.
View full profile and credentials →Take a look at the financing options
Don’t worry, we’ll take care of everything!